Carotid Artery Disease Treatment Memphis TN
Understanding Carotid Artery Disease: Symptoms and Warning Signs
Carotid artery disease is a condition characterized by the narrowing or blockage of the carotid arteries. These arteries are located in the neck and are responsible for supplying blood to the brain. This condition can have significant implications for cardiovascular health and overall well-being.
At Zenith Vascular & Fibroid Center, we proudly offer a range of Carotid Artery Disease treatment options. Learn more during a consultation with us in Memphis, TN!
What is Carotid Artery Disease?
Carotid artery disease refers to the narrowing or blockage of the carotid arteries, which are the major blood vessels supplying oxygen-rich blood to the brain. The symptoms of carotid artery disease may vary depending on the severity of the blockage and the extent to which blood flow is compromised.

Risk Factors
Carotid artery disease is a condition where the carotid arteries, which supply blood to the brain, become narrowed or blocked due to the buildup of plaque. Several risk factors can contribute to the development of carotid artery disease. Here are some common risk factors to be aware of:
1. Age: As age increases, the risk of developing carotid artery disease also increases. The risk is higher in individuals over the age of 65.
2. Gender: Men have a higher risk of developing carotid artery disease compared to pre-menopausal women. However, after menopause, women’s risk catches up to that of men.
3. Family History: Having a close family member, such as a parent or sibling, with a history of carotid artery disease increases your risk. Genetic factors can play a role in the development of the disease.
4. Smoking: Smoking damages the blood vessels and promotes the formation of plaque, increasing the risk of carotid artery disease. We highly recommend quitting smoking as soon as possible.
5. High Blood Pressure: Uncontrolled high blood pressure puts extra strain on the blood vessels, promoting the development of plaque and increasing the risk of carotid artery disease.
6. High Cholesterol: Elevated levels of LDL (bad) cholesterol and triglycerides can lead to the formation of plaque in the arteries, including the carotid arteries.
7. Diabetes: People with diabetes are at a higher risk of developing carotid artery disease due to the increased likelihood of having other risk factors such as high blood pressure and high cholesterol.
8. Obesity and Sedentary Lifestyle: Being overweight or obese, as well as leading a sedentary lifestyle, increases the risk of carotid artery disease.
9. Unhealthy Diet: Consuming a diet high in saturated and trans fats, cholesterol, salt, and sugar increases the risk of carotid artery disease. A diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can help reduce the risk.
10. History of Heart Disease: Individuals with a history of heart disease, such as a previous heart attack or coronary artery disease, are at a higher risk of developing carotid artery disease.
It is worth noting that these risk factors can be managed and modified. By adopting a healthy lifestyle, such as quitting smoking, maintaining a healthy weight, engaging in regular physical activity, following a balanced diet, managing blood pressure, cholesterol, and diabetes, you can significantly reduce your risk of carotid artery disease and improve your overall cardiovascular health. Regular check-ups and screening tests can also help detect the disease in its early stages. If you have any concerns or risk factors, it is important to consult with a healthcare professional for personalized advice and guidance.
How is Carotid Artery Disease diagnosed?
Carotid artery disease can be diagnosed through various methods that help assess the degree of narrowing or blockage in the carotid arteries. Here are some common diagnostic tests and procedures used:
1. Physical Examination: A healthcare professional may perform a physical examination, including listening for carotid bruits with a stethoscope placed over the neck. While a carotid bruit does not directly diagnose carotid artery disease, it can indicate the presence of abnormal blood flow.
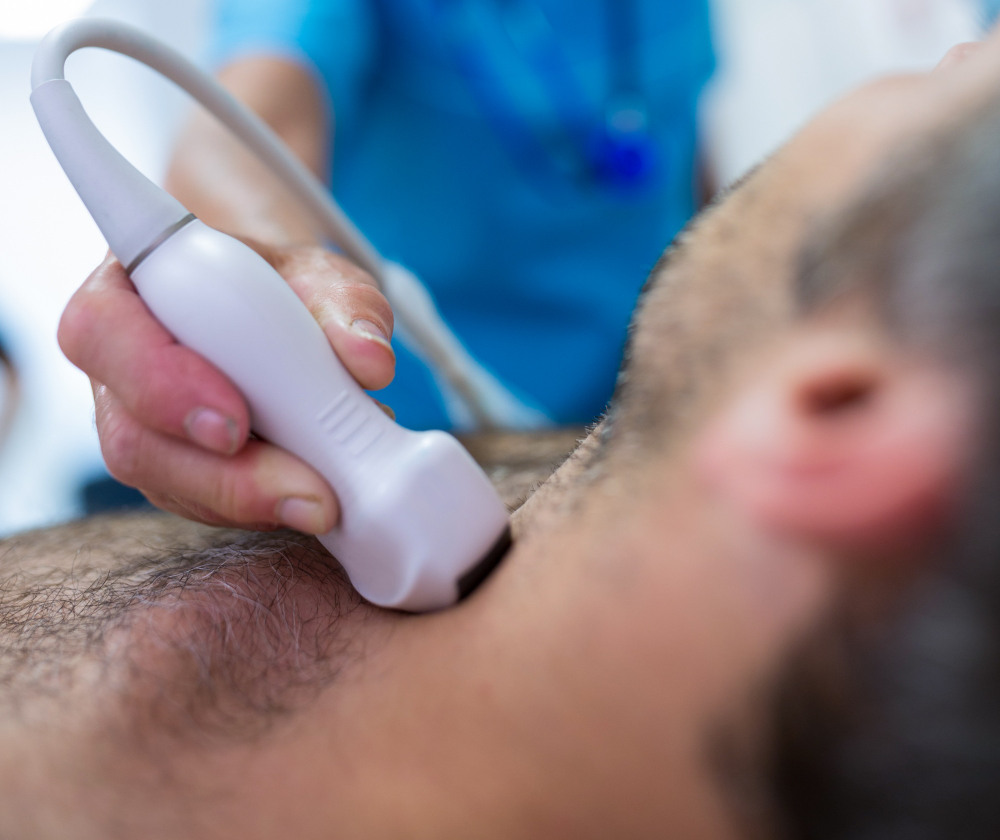
2. Carotid Doppler Ultrasound: This non-invasive test uses sound waves to create images of the carotid arteries. It can assess the blood flow through the arteries, detect any narrowing or blockages, and determine the severity of the condition.
3. Computed Tomography Angiography (CTA): This imaging technique combines a series of X-ray images to create detailed cross-sectional images of the carotid arteries. It can provide information about the extent of plaque buildup and the presence of any blockages.
4. Magnetic Resonance Angiography (MRA): MRA uses magnetic fields and radio waves to create detailed images of the carotid arteries. It provides information about blood flow and can help identify any narrowing or blockages.
5. Digital Subtraction Angiography (DSA): DSA is an invasive procedure where a contrast dye is injected into the bloodstream, followed by X-rays to visualize the carotid arteries. It provides detailed images of the blood vessels and can precisely identify the location and severity of blockages.
6. Transcranial Doppler (TCD): TCD is a non-invasive test that uses sound waves to evaluate blood flow within the brain’s blood vessels. It can help assess the presence of blood clots or other abnormalities related to carotid artery disease.
7. Blood Tests: Blood tests may be performed to assess cholesterol levels, blood sugar levels, and other factors that can contribute to carotid artery disease.
It is important to consult with a medical professional if you suspect or have risk factors for carotid artery disease. At Zenith Vascular & Fibroid Center, we will evaluate your medical history, perform a physical examination, and recommend appropriate diagnostic tests based on your symptoms and risk factors. Early detection and accurate diagnosis are crucial for timely intervention and management of carotid artery disease to prevent complications such as stroke.
What treatments are available for carotid artery disease?
There are several treatment options available for carotid artery disease, and the choice of treatment depends on the severity of the disease, the presence of symptoms, and individual patient factors. Here are some common treatment approaches:
1. Lifestyle Modifications: Making healthy lifestyle changes can be an essential part of managing carotid artery disease. This includes adopting a heart-healthy diet low in saturated fats and cholesterol, engaging in regular physical activity, maintaining a healthy weight, managing blood pressure and blood sugar levels, and quitting smoking.
2. Medications: Medications may be prescribed to manage carotid artery disease and associated risk factors. These may include antiplatelet medications (such as aspirin or clopidogrel) to prevent blood clots, cholesterol-lowering medications (such as statins) to control high cholesterol levels, blood pressure medications, and medications to manage diabetes.
3. Carotid Endarterectomy: This surgical procedure involves the removal of plaque from the carotid artery. It is typically performed when there is a significant narrowing of the artery (usually greater than 70%) or when symptoms are present. By removing the plaque, blood flow to the brain is improved, reducing the risk of stroke.
4. Carotid Angioplasty and Stenting: This minimally invasive procedure involves inserting a catheter with a balloon into the narrowed carotid artery. The balloon is inflated to widen the artery, and a stent (a small mesh tube) is placed to keep the artery open. This procedure is an alternative to carotid endarterectomy, particularly for patients who are considered high risk for surgery.
Early diagnosis and management of carotid artery disease is crucial to prevent complications such as stroke. Regular follow-up with a healthcare professional is important to monitor the progression of the disease and adjust treatment as necessary.
What do doctors recommend to patients after an endarectomy?
After an endarterectomy, doctors typically recommend several things to patients to promote healing and reduce the risk of complications. Here are some common recommendations:
1. Medications: Patients may be prescribed medications to prevent blood clots and manage other risk factors. This may include antiplatelet drugs (such as aspirin) or anticoagulants, which help prevent the formation of new blood clots.
2. Pain management: Patients may be given pain medication to manage any discomfort or pain following the procedure. It’s important to follow the prescribed dosage and instructions for pain relief.
3. Wound care: Proper wound care is crucial to prevent infection and promote healing. Patients will be advised on how to clean and care for the incision site, including instructions on changing dressings and keeping the area clean and dry.
4. Physical activity: While rest is important initially after the procedure, doctors generally encourage patients to gradually resume physical activity. It’s important to follow the specific guidelines provided by the healthcare team. Gentle exercises and walking may be recommended to help improve blood flow and aid in recovery.
5. Diet and lifestyle modifications: Doctors often recommend making healthy lifestyle changes to manage underlying risk factors. This may include adopting a balanced diet low in saturated fats and cholesterol, maintaining a healthy weight, engaging in regular exercise, and quitting smoking if applicable.
6. Follow-up appointments: Patients will need to schedule and attend follow-up appointments with their healthcare team. These appointments are essential for monitoring progress, managing medication, and assessing overall recovery.
It’s important for patients to adhere to these recommendations and communicate any concerns or questions with their healthcare provider to ensure a smooth and successful recovery.

Prevention Tips for Carotid Artery Disease
Carotid artery disease is a condition characterized by the narrowing or blockage of the carotid arteries. These arteries are located in the neck and are responsible for supplying blood to the brain. This condition can have significant implications for cardiovascular health and overall well-being.
Regular exercise is crucial for maintaining cardiovascular health and can play a significant role in preventing or managing carotid artery disease. Engaging in physical activity helps to improve blood flow, reduce plaque buildup, and strengthen the heart muscles.
In some cases, surgical interventions may be necessary to address severe cases of carotid artery disease. Two common procedures used for treatment are carotid endarterectomy and stenting. Carotid endarterectomy involves removing plaque from the affected arteries, while stenting involves placing a small mesh tube called a stent to keep the artery open.
If you are seeking treatment for carotid artery disease in Memphis TN, it is important to consult with a qualified vascular surgeon who specializes in this area. A vascular surgeon will assess your specific condition and recommend appropriate treatment options based on your individual needs.
Overall, understanding what carotid artery disease is and how it develops is crucial for individuals looking to maintain their cardiovascular health. By incorporating regular exercise into their routine and seeking appropriate medical interventions when necessary, individuals can take proactive steps towards managing this condition effectively.
Patient Education
Zenith Vascular is committed to helping patients navigate their care journey. This list of resources is intended to help patients, caregivers & advocates address some of the questions and challenges that come up in managing vascular healthcare.
Understanding the Vascular System
Your vascular system – the highways of the body – is composed of three types of blood vessels.
Veins
Veins are a type of blood vessel that carry deoxygenated blood from the body’s tissues back to the heart. They work in conjunction with arteries, which carry oxygenated blood away from the heart and toward the body’s tissues.Veins have thin walls compared to arteries and rely on surrounding muscles to help push the blood back toward the heart.
Veins also have one-way valves that prevent blood from flowing backward. When these valves function properly, they help ensure that blood flows in one direction only, toward the heart. If these valves become damaged or weakened, blood can start to flow backward, causing the veins to become swollen and twisted.
Arteries
Arteries are blood vessels that carry oxygenated blood away from the heart and toward the body’s tissues. They play a crucial role in maintaining the body’s blood flow and ensuring that oxygen and nutrients are delivered to all of the body’s organs and tissues. Arteries have thick, muscular walls that allow them to withstand the high pressure of blood flow that is generated by the heart’s pumping action.
Arteries can become damaged or narrowed due to a variety of factors, including smoking, high blood pressure, high cholesterol, and diabetes. This can lead to conditions such as atherosclerosis, which is a buildup of plaque in the arteries that can restrict blood flow and increase the risk of heart
Capillaries
Capillaries are the smallest and thinnest blood vessels in the human body. Capillaries are found throughout the body, and their extensive network ensures that every cell in the body is supplied with the oxygen and nutrients it needs to function properly. When blood flows through the capillaries, oxygen and nutrients diffuse out of the blood and into the surrounding tissues, while waste products such as carbon dioxide diffuse from the tissues into the blood.
Capillaries are also a key site for the delivery of oxygen and nutrients to the body’s muscles during exercise. Capillaries can be damaged by a variety of factors, including high blood pressure, diabetes, and inflammation.
